Challenge Statement
While there are data exchange standards in place to share information between individual state PDMPs (also called PMPs) and standards to exchange information between Health IT System( eg. EHR, HIE (removed based on further clarification in the Use Case) , Pharmacy) there are no widely adopted standards for the flow of data from a PDMP to a Health IT System. As PDMP systems have evolved outside the health IT ecosystem, significant barriers to interoperability have resulted. One of the current technical barriers to interoperability is the lack of standard methods to exchange and integrate the prescription drug data available in PDMPs into health IT systems . There are a lack of common technical standards and vocabularies to enable PDMPs to share computable information with the health IT system that providers can use to support clinical decision-making.
To achieve interoperability, consistent and standardized electronic methods need to be established to enable seamless and secure data transmission between PDMPs and health IT systems.
Background
Prescription drug misuse and overdose is one of the fastest growing health epidemics in the United States. One of the most promising clinical tools to address prescription drug abuse are prescription drug monitoring programs (PDMPs). PDMPs are state-run electronic databases – functioning in 48 U.S. states and territories – that track the prescribing and dispensing of controlled prescription drugs to patients.
Information within PDMPs is intended to enhance health care professionals' (e.g. physicians, pharmacists, dispensers, delegated authorities with legal authorization) understanding of their patients’ controlled substance history. While health care professionals see PDMPs as a valuable tool, they often do not use PDMPs because they are “stand alone” systems which are cumbersome and time consuming to access. When available at the point of care and point of dispensing, PDMP information can help health care professionals discern between patients who may need a controlled substance for legitimate medical treatment and those who may be seeking to misuse prescription drugs. It also provides an opportunity to intervene if there are signs of misuse and abuse. In some states health care professionals are required to check the PDMP prior to dispensing controlled substances. This underscores the need for PDMPs to share information with health IT systems in ambulatory and acute care settings.
Currently, many health care professionals must either interrupt their workflow and log on to a separate system to access the PDMP, or write and dispense prescriptions without consulting the PDMP- potentially leaving health care professionals without the information needed to make important clinical decisions. One way to improve and encourage PDMP access is to reduce the number of steps it takes to access the PDMP. Health IT systems can accomplish this by querying PDMPs for prescription information and presenting this information to health care professionals when they access a patient’s health record.
Purpose and Goals
The purpose of this initiative is to bring together the PDMP and health IT system communities to standardize the data format, transport, and security protocols to exchange patient controlled substance history information between PDMPs and health IT systems. Doing so would enable health care professionals to make more informed clinical decisions through more timely, effective and convenient access to PDMP data in an effort to reduce prescription drug misuse and overdose in the United States. The specific goals are:
- Define use case requirements and implementation guide to securely and appropriately communicate patient controlled substance data from PDMP to HealthIT system
- Identify existing stakeholders and methodologies for accessing PDMP data.
- Identify, evaluate, and harmonize the data format(s) sent from PDMPs to Health IT systems
- Define standard transactions between the HealthIT system and the PDMP
- Identify standards that allow the Health IT system the ability to query the PDMP
- Identify gaps in selected standards and work with standards organizations to fill in those gaps
- Evaluate and select transport protocol(s) systems support.
- Evaluate and select security protocol(s) systems support.
Scope Statement
To allow system integrations that arm health care professionals with legal authorization with PDMP data as part of their normal clinical workflow by:
- Connecting PDMPs to health IT systems using existing standards; (technical mechanism for actual exchange of data)
- If standards do not exist, identifying the gap in the current standards and working with the Standards Organizations (SDOs) to address the gaps
- Improving effective and efficient access to PDMP data by health care professionals
Out of Scope
- Defining the trigger event for how the PDMP is queried or initiated by the user (e.g., hyperlink while ordering, pressing a button, automatic trigger, etc.)
- Addressing delegation of rights to individuals not legally authorized to prescribe medications (this is an implementation specific decision and may vary by implementation and pilot sites)
- PDMP to PDMP transactions (State to State)
- Third party access - (this is an implementation specific decision and may vary by implementation, pilot sites and state statues and law)
- Reporting patient prescription information from dispensers to state PDMP
Value Statement
- The feedback received from health IT community between PDMP and healthIT systems will influence data format, application programmatic interface, and transport protocol for interfaces for querying data from PDMP instances;
- The outcome will be a specification describing the data interface for querying prescription information from a PDMP instance for use by health IT systems which enables
- The ability for Health Care Professionals with legal authorization to access prescription drug data for patients at the point of care to make informed clinical decisions and appropriate treatment recommendations to reduce prescription drug misuse and overdose
Potential Standards for Consideration
Note – The below standards are a starting list for consideration and will be updated based on community feedback during Charter discussions and as use case requirements are further fleshed out. This is not a full list of all possible standards.
- Content and Structure: C32, CDA R2, FHIR, HL7 V.2.X, XML, NCPDP SCRIPT, ISO 32000-1:2008
- Transport and Security: NCPDP SCRIPT, hData, SOAP, ASAP Webservices, XDR and XDM (Direct), NCPDP Telecommunication, REST
- Other: NIEM IEPD, PMIX
- Other references: NarxCheck, OpenSearch, Rcopia, RHEx, RPC, Surescript, Zero Report Standard (by ASAP)
- Vocabulary Standards: RxNorm, National Drug Code (NDC)
Potential Risks
- Privacy and Security: If data is intercepted en route between a PDMP and a Health IT System, patient confidentiality may be compromised.
- Mitigation: Employ secure protocols to encrypt and protect data in transit and prevent unauthorized disclosure.
- Unintended access to data not requested by the prescribers
- Patient mismatch
- Financial challenges of a new standards requirement
- It is possible that some approaches presented in the Use Case may require state regulatory approval or modification
Stakeholders
- Prescription Drug Monitoring Programs
- Prescription drug prescribers
- Prescription drug dispensers
- Health Care Professionals (Healthcare providers with patient care responsibilities such as; physicians, Advanced Practice Registered Nurses, Physician Assistants, nurses, pharmacists, emergency care providers, behavioral health team members, care coordinators and other patient care personnel) who may access the PDMP during the course of providing care.)
- Patients and patient advocates
- EHR/EMR vendors
- State HIEs
- Local, State, Federal Government
- Trade Associations
- Professional Associations (AMA, Pharmacy Associations)
- PDMP Application Vendors
- Standards Organizations
- Healthcare Payers
- Third party organizations
Consensus
<iframe width='760' height='500' frameborder='0' src='https://docs.google.com/spreadsheet/pub?key=0ApW4Ox66ml2IdHR6aW9LcWpYQVlhbE95eEotNU1lX1E&output=html&widget=true'></iframe> |
End to End Review
<iframe width='700' height='500' frameborder='0' src='https://docs.google.com/spreadsheet/pub?key=0ApW4Ox66ml2IdGNJaGxQOURKT19qZXlKS1gwWnhyZkE&output=html&widget=true'></iframe> |
Members
<iframe width='400' height='500' frameborder='0' src='https://docs.google.com/a/siframework.org/spreadsheet/pub?key=0ApW4Ox66ml2IdGxIczh1VmJaNDBJUGtOd2R1SktIelE&output=html&widget=true'></iframe> |
Timeline
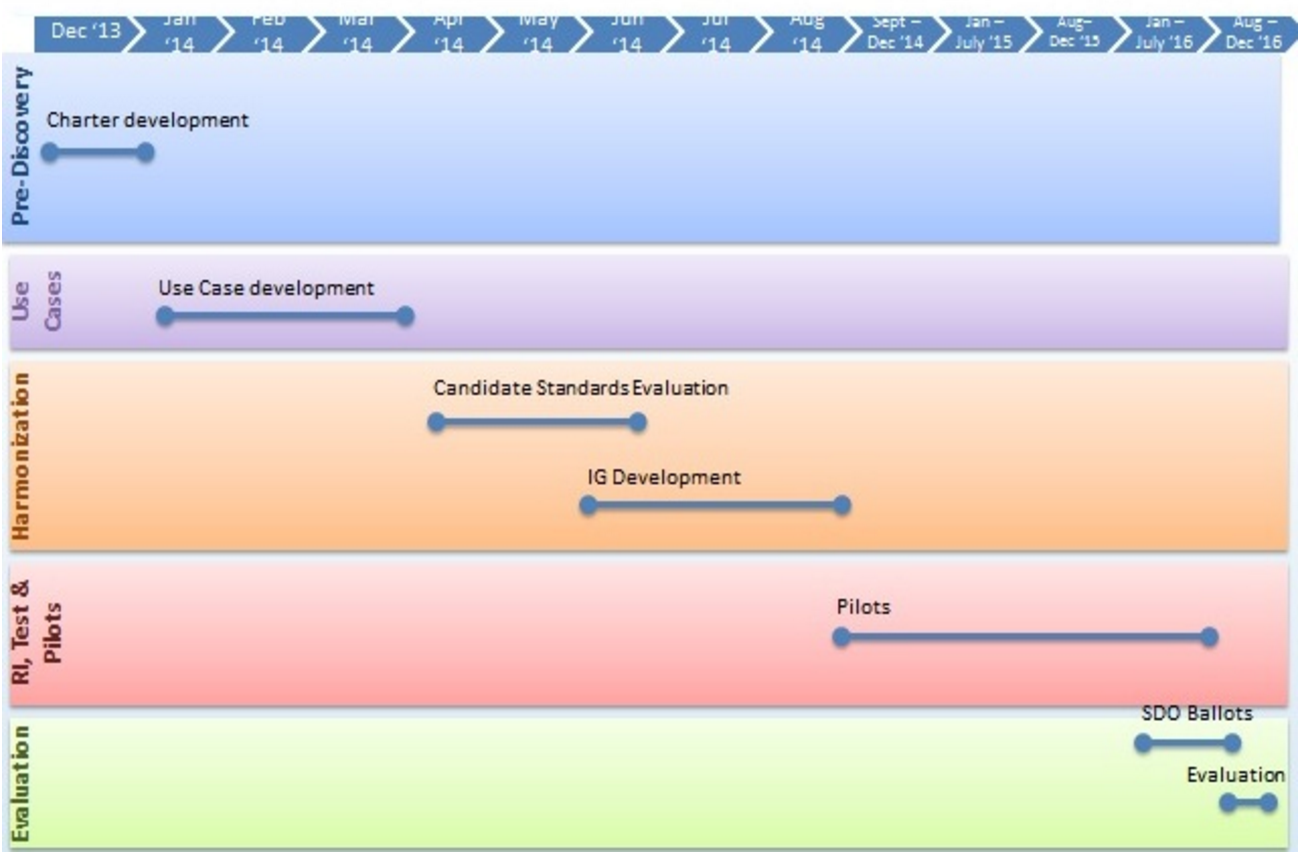
Initiative Contacts
| Name | Role | |
|---|---|---|
| Johnathan Coleman | Initiative Coordinator | jc@securityrs.com |
| Sherry Green | PDMP SME | sgreen586@gmail.com |
| Mera Choi | ONC Lead | mera.choi@hhs.gov |
| Jennifer Frazier | ONC Lead | Jennifer.Frazier@hhs.gov |
| Helen Caton-Peters | ONC Lead | Helen.Caton-Peters@hhs.gov |
| Tricia Lee-Wilkins | ONC Lead | Tricia.Wilkins@hhs.gov |
| Jinhee Lee | SAMHSA Lead | Jinhee.Lee@samhsa.hhs.gov |
| Kate Tipping | SAMHSA Lead | Kate.Tipping@samhsa.hhs.gov |
| Jamie Parker | Project Management | jamie.parker@esacinc.com |
| Saurav Chowdhury | Project Support | saurav.chowdhury@esacinc.com |
| Taima Gomez | Project Support | taima.gomez@esacinc.com |